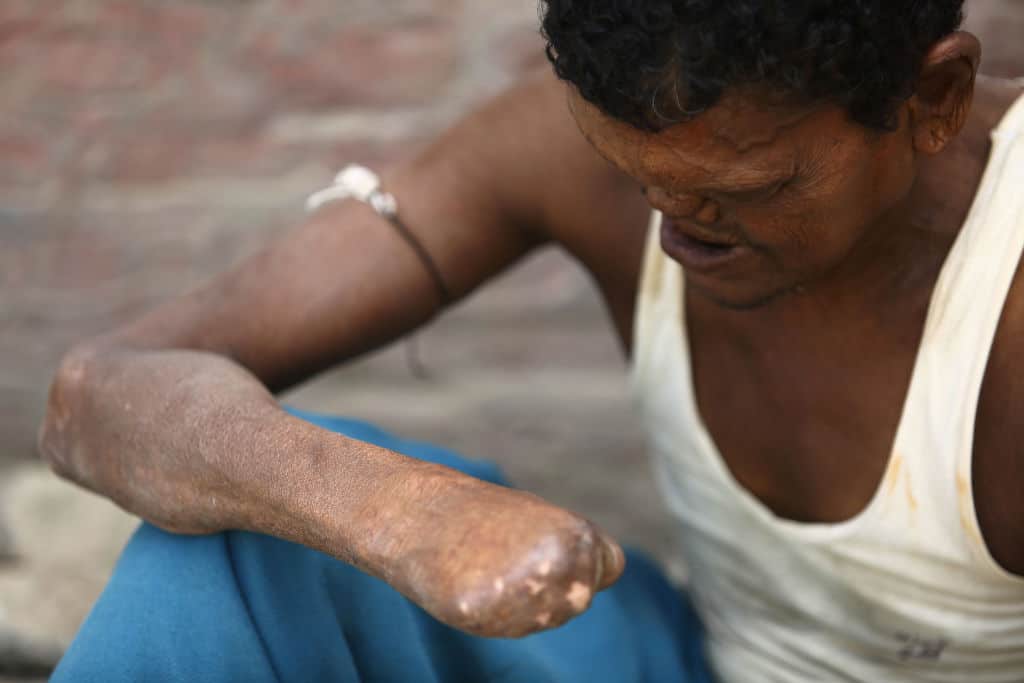
Leprosy has been a death sentence for most of human history. Before the disease kills the one who suffers, it frequently means exile for sufferers from home and community. So much so, that ‘leper’ long ago became a cruel byword for someone to be avoided.
In much of the world, the malady is known these days by a different name: Hansen’s disease, after the Norwegian scientist Gerhard Henrik Armauer Hansen, who discovered the bacterium that causes the illness. Medicine has made significant strides in understanding the disease and developing treatments, while public health professionals have come to understand how to control its spread. Leprosy cases are dropping worldwide, and many countries especially in the developed world have declared the disease eliminated.
It’s not all rose-coloured, though – not by a long shot.
There are two main problems.
The slow onset of the disease and the particular vulnerability to it of poor people already living at the margins of society mean that people frequently go undiagnosed until it is too late, and then struggle to find help when they need it most.
Also, governments and citizens in the developed world are largely unaware of the problem’s scope, gravity, or persistence; while leaders, caregivers, public health officials and even sufferers themselves in nations where the disease still ravages populations continue to labour under the debilitating weight of misconception; that leads to stigma, needless and unjust discrimination, and exclusion from society that all perpetuate a vicious cycle.
For a disease to be “eliminated”, as some governments claim leprosy has been, fewer than 1 in 10,000 people must suffer it. But in vast populous countries in the poorer parts of the world, the designation hides a still considerable problem. In India, which has a population of nearly 1.4 billion, there are 130,000 new cases of leprosy year.
With the apparent disappearance of the disease in Europe and the US (there were only 139 new cases in the UK between 2003 and 2012), the reality of leprosy in the developing world goes unheeded.
The St Francis Leprosy Guild (SLFG) is a charity pushing back against indifference – and punching well above its weight in the fight to prevent, cure, and treat the disease itself. SFLG have cared for people with leprosy for 125 years, and believe an end to leprosy worldwide is possible within a lifetime.
They also say that lack of real understanding on the part of leaders at every level of society both in the developed and the developing world risks missing millions of people, who go undiagnosed until it is too late.
The keys are education, better public health practices – for which the tip of the spear is a method called Active Case Finding – and funding.
The stigma against those with leprosy frequently leaves sufferers on the margins of society, living in impoverished conditions with unreliable access to running water and hygiene facilities. Compounded if they have also suffered from Covid-19, particularly if a family member has died, leprosy it frequently prevents them or their family from pursuing or receiving medical assistance, which is in itself not forthcoming from societies weary of leprosy.
There are 130 laws worldwide specifically discriminating against those with leprosy – 106 of which are in India, where people who have leprosy cannot be elected to local government, use public transport, go to school, or even borrow books from public libraries. In some Indian states, it is grounds for divorce.
And while leprosy can be treated and the worsening of symptoms halted, the disfigurement and disabilities brought on by the disease are lifelong – even those cured of the disease suffer at the hands of legal and social prejudice.
However, the St Francis Leprosy Guild are confident zero leprosy is possible by pursuing Active Case Finding (ACF).
ACF is a door-to-door approach, where well-trained teams go out into a community to test everyone for signs of the disease. The skin and the peripheral nervous system – the relay between the brain and the limbs and organs – are tested for signs of leprosy, often presenting as an inability to feel pain or a loss of sensation.
Much like the test and trace systems governments worldwide introduced to tackle the spread of Covid-19, anyone who has come into contact with a case of leprosy is tracked down and tested.
If a contact shows signs of leprosy, they can be treated with multidrug therapy – freely available from the World Health Organization, which prevents the severest symptoms of the disease from taking effect. A single dose preventative shot is given to any contact not displaying symptoms.
Though ACF is already in place, it doesn’t come cheap. In countries that have “eliminated” leprosy and redirected resources accordingly, the much-needed and sizeable funds for training teams and getting them to often remote communities are not forthcoming.
The “double-discrimination” of leprosy and Covid-19 has made it all the harder for those with leprosy. Already struggling to pursue or receive medical and food assistance due to the discrimination that they face, advocates fear that they are at the back of the queue for the vaccine.
“People with leprosy would be the last people on earth to receive a Covid-19 vaccine and people with leprosy AND Covid-19 suffer the injustice of ‘double-discrimination’. We need proactive Covid-19 vaccine support for the leprosy community here,” said Arun Kuma, the program manager at the Leprosy Mission outside New Delhi.
The added isolation of the pandemic has, “left them with nothing,” he said. “They have to beg to survive.”
As the pandemic has progressed, governments have been called on to act by senior clergy and charities alike to ensure fair distribution of the vaccine to the most marginalised groups across the globe. And as the British government alone has ordered 407 million doses of the vaccine from 7 different companies, it is expected and has indeed been requested that they donate them to poorer countries, once the UK is fully vaccinated.
The SFLG, which helped 77,000 people with the disease over the past year and runs centres across the world in countries such as India, Liberia and Brazil, has a longstanding relationship with the Catholic Church in England and Wales. All of the Bishops of England and Wales are patrons of SFLG. However, SFLG maintains a particularly close relationship with the archdiocese of Southwark in London.
Last week, Archbishop John Wilson of Southwark urged the UK to pursue this policy of vaccine equity. “We know from the experience of the Covid-19 pandemic in the United Kingdom that protecting the health and wellbeing of the most vulnerable is a priority,” said Archbishop Wilson. “As soon as vaccines against Covid-19 are available to every country, it is vitally important that disadvantaged communities, such as those affected by leprosy, are enabled to receive the same benefits from vaccination as the rest of society.”
As those with leprosy often live isolated from the rest of society, in cramped and impoverished conditions, advocates have proposed that governments define strategies to tackle the issues facing those who have the disease.
Director of the SFLG, Clare McIntosh said, “It is important that governments have specific strategies in place to ensure that disadvantaged communities benefit from the same outcomes of Covid-19 vaccines as everyone else.”
McIntosh noted that some cities are making vaccines available to vulnerable communities using mobile clinics, which enables people who live in remote locations or in any case have a hard time traveling to receive the Covid-19 vaccine.
A fraction of the funding put into Covid-19 research and treatment could go a very long way, indeed, to serve the cause of really ending leprosy once and for all.
![]()
This page is available to subscribers. Click here to sign in or get access.
Areas of Catholic Herald business are still recovering post-pandemic.
However, we are reaching out to the Catholic community and readership, that has been so loyal to the Catholic Herald. Please join us on our 135 year mission by supporting us.
We are raising £250,000 to safeguard the Herald as a world-leading voice in Catholic journalism and teaching.
We have been a bold and influential voice in the church since 1888, standing up for traditional Catholic culture and values. Please consider donating.



